In life, you have to have opinions. Not just internal monologue, but true spoken opinions. And if they matter enough, you need conviction behind them.
So here's mine: after learning the inner workings of health insurance for mid-market companies and partnering with some of the most innovative companies in the space, my opinion is this: the fully insured model shouldn't be the default answer.
Small companies stay on small group benefits or a PEO. Enterprise companies self-fund and have dedicated teams to manage their strategy and performance. Mid-sized employers are stuck in an ugly middle zone, one called fully insured, which feeds extraordinary profits to everyone who touches their benefit plans. The dirty little secret in the benefits advisory world is that you can make up to 10x more money on a fast-growing mid-sized company than you would servicing an enterprise on a flat fee. Since both carriers and brokers make significantly more on fully insured plans, the strategy writes itself: find a growing company, set up large group fully insured plans, build a moat around it through bundled wellness programs, software, and branded "programs," and keep it as comfortable as possible for as long as possible. That's how brokers and carrier reps get rich.
So what are the other options for mid-sized employers? You could stay on a PEO, but the admin fees become astronomical at scale. You could set up a stipend so employees can buy insurance on individual markets, but this is highly state-dependent, puts the burden on employees to navigate a catalog of plans, and ultimately just kicks the can down the road. You could move directly to self-funding, but at smaller sizes, one or two high claimants can blow up the entire plan. There is one other option, so criminally underutilized that most people probably aren't even thinking about it.
That option is an employee benefits group captive. It allows mid-sized employers to effectively join a pooled self-funding program. It's typically structured in three layers: a self-funded layer, where the employer pays for low-cost medical expenses directly; a shared layer, where employers pool money to cover mid-sized claims together; and an excess layer, where a premium is paid to cover large, unpredictable claims.
I spent the last few months entirely dedicated to understanding the group captive landscape. The structural case is sound. The real question is how to navigate a market that hasn't fully caught up to its potential yet.
The Structural Case Is Sound
The most important thing captives get right is something that sounds almost obvious once you hear it: pay for what is predictable, and insure what is not.
Roughly 80% of claims for a mid-sized organization are low-cost and can be predicted at the aggregate level with a high degree of accuracy. The fully insured model has convinced employers to insure those expenses anyway, which means paying a margin north of 20% on costs that carry essentially no risk.
That margin, applied to 80% of your claims, adds roughly 16 points to your total healthcare spend. That is 16% of a multi-million dollar annual expense that is mostly waste.
The analogy I keep coming back to: imagine adding gas coverage, oil changes, car washes, and tire rotations to your auto insurance policy, with a copay. You can predict with reasonable accuracy what you will spend each year to keep a car running. What you cannot predict is a collision, a total loss, a one-time event that creates genuine financial exposure. You pay for the routine, and insure the unpredictable. That logic holds consistently across virtually every other form of insurance. Health benefits are the exception, and employers have been absorbing the cost of that exception for decades.
Captives correct this. They allow smaller employers to safely enter self-funding earlier, removing most of the waste on the 80% of predictable spend and, importantly, taking back control of their data.
What the Numbers Actually Look Like
But captives today usually don't boast expected savings of 16% savings in year 1. So, I analyzed the financials of more than ten captive programs. The goal was simple: understand where the theoretical savings are going, and what employers are actually capturing today.
The theoretical case is clean. Remove the carrier margin on predictable spend, pool the mid-tier risk, insure the catastrophic tail, and you should see immediate meaningful savings. The market has not fully delivered on that yet. Here is why.
Stop-loss carriers double-dip. They take heavy fees for fronting carrier duties required for the captive to hold risk in the middle layer, and they charge opaque fees on the excess layer as well. Professional Captive Managers charge heavily for compliance and back-office functions baked into the plan. Captive Program Managers, particularly larger ones, charge a small PEPM management fee while also pulling revenue through three or four other streams that directly inflate cost. TPAs are essential for claims management and genuinely valuable, but they cost more than ever. And your broker still needs to be paid.
The captive layer itself typically carries around 25% in pure expense load, on top of $25 to $45 per employee per month to insure the excess layer. Leaner programs tend to run total friction costs around 10% of the total plan. Larger programs often land closer to 15-20%. Once you layer in TPA fees, broker compensation, and additional vendor costs, the all-in expense structure frequently approaches the fully insured equivalent premium before any underwriting surplus is returned.
But this is precisely the point. In a fully insured plan, that is where the story ends. In a captive, what comes next is what matters: you receive surplus returns from your own self-funded performance and from the captive pool, you own your data, and your leverage over costs compounds every year you stay in the structure. The gross program cost before surplus looks similar to fully insured. Everything after that is different.
The majority of savings come from expected surpluses, both in your own self-funded performance and in the captive layer itself. Your self-retained layer has a per-claim deductible sized to your organization, calibrated to capture the low-cost, predictable claims that should never have been insured in the first place. Aggregate stop-loss protects you in bad years, typically kicking in when total claims exceed 120% of what was expected. This means your self retained responsibility is largely predictable and protected against anomalous years. This layer of spend is now highly efficient because the carrier margin that normally sits on top of this layer is largely removed. You are simply paying for what you use, without the excessive overhead.
The captive layer, while heavily expensed, adds a second source of return. Most programs target an annual surplus of around 8%. But how certain that return is, and how wide the range of outcomes around it can be, depends heavily on one variable that most people underweight: the size of the pool you are in.
Pool Size Changes the Risk Profile Entirely
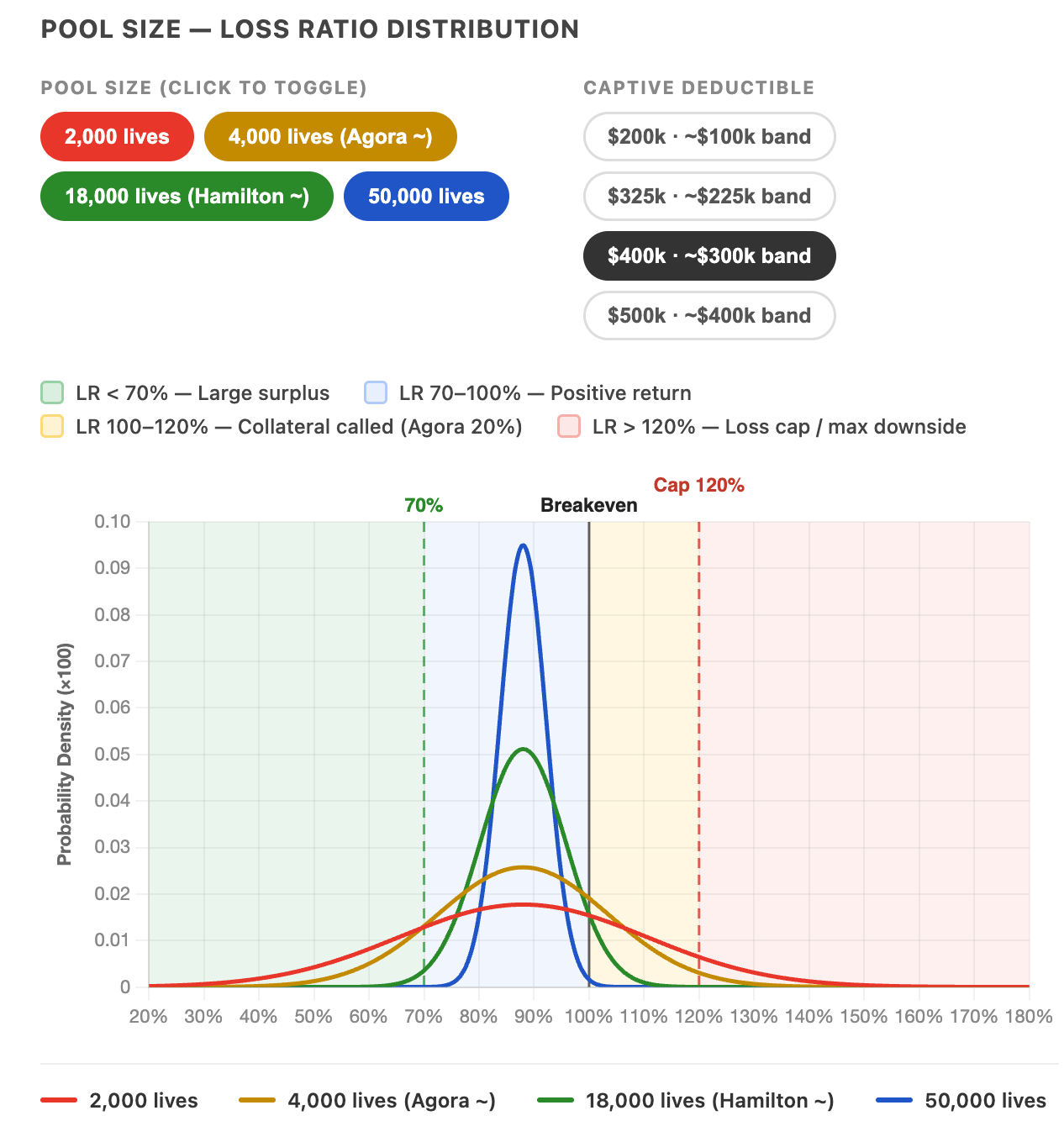
A captive with 18,000 lives operates in an almost entirely different risk environment than one with 2,000. At large pool sizes, outcomes converge tightly around the expected mean. A 50,000-life pool produces a surplus in roughly 98% of years. The risk is negligible. Unfortunately, so is the potential for an exceptional outcome.
Smaller pools carry real variance, and the structure of a captive makes that variance asymmetric in the employer's favor. The worst case in any captive is a full capital call, typically 20% of ceded premium. That is the floor, and it is fixed. At a 2,000-life pool, the probability of a genuinely large surplus year is close to 16%. At 4,000 lives, it's 8%. At 50,000 lives, it's .1%. The worst case is capped at the same level in every pool, but smaller pools have real probability of exceptional years that large pools cannot produce.
When the distribution is tight, as it is at 50,000 lives, you are effectively paying heavy overhead and risk margin to a captive that takes very minimal risk. Scale that to over 1 million lives, which is what the largest group captive operates at, and the distribution becomes essentially predictable. You end up with fully insured redundancy. Different players collecting the margin. That stability matters for groups that need it. But high performers are paying for a protection they aren't using.
In smaller group captives, the demographics of your pool-mates matters much more. The composition of the businesses in these programs directly affects the distribution of outcomes and the stability of the program over time. It is a critical piece of due diligence that does not get enough attention.
The Real Advantage Is Your Data
The immediate financial argument gets most of the attention, but it is not the most durable part of the case for captives.
When you move to a captive or any self-funded structure, you own your claims data. You can see what is driving cost, identify members heading toward high-cost episodes before they arrive, and build a proactive strategy instead of reacting to whatever renewal number your carrier presents each fall.
In a fully insured environment, that data stays with the carrier. It is used to serve their underwriting interests, not yours. Major carriers are vertically integrated businesses. Their underwriting profits are capped by regulation, which means growth requires premiums to rise or additional margin to be extracted through pharmacy operations, network management, and other integrated services. They are not structurally positioned to lower costs for employers, and expecting them to do so voluntarily is hopeful to say the least.
Access to your data changes the game completely. And when you partner with an experienced TPA, you can understand what your population actually needs, direct members toward high-value care before a routine condition becomes a catastrophic one, and measure the ROI of every cost containment dollar you spend.
This is also where the mindset shift matters most. Fully insured trains employers to think in one-year cycles. You get a renewal number, you negotiate, you sign, you repeat. There is no mechanism for building on last year's work because you do not own last year's information. A captive inverts that. Year two is better than year one because you have a year of your own data. Year three is better than year two because you have started acting on what you learned. The cost containment programs you implement in year one produce results that show up in year two's claims. The high-cost member you identify and route to a center of excellence in year two avoids a catastrophic episode in year three. That compounding does not happen in a fully insured model. It cannot, because the structure does not allow it.
Moving to a captive opens the door for smaller employers to a fundamentally different model for managing health spend, and the payoff builds every year you stay in it.
Who Is Not in the Room
Going through the demographics of various captive pools, I noticed something worth calling out. The west coast and the technology industry are significantly underrepresented. Some of that is regulatory: California has real complexity. But the pattern holds well beyond any single state. The captive world has traditionally skewed toward manufacturing, wholesale, and industries with historically higher physical risk profiles. Technology is largely absent.
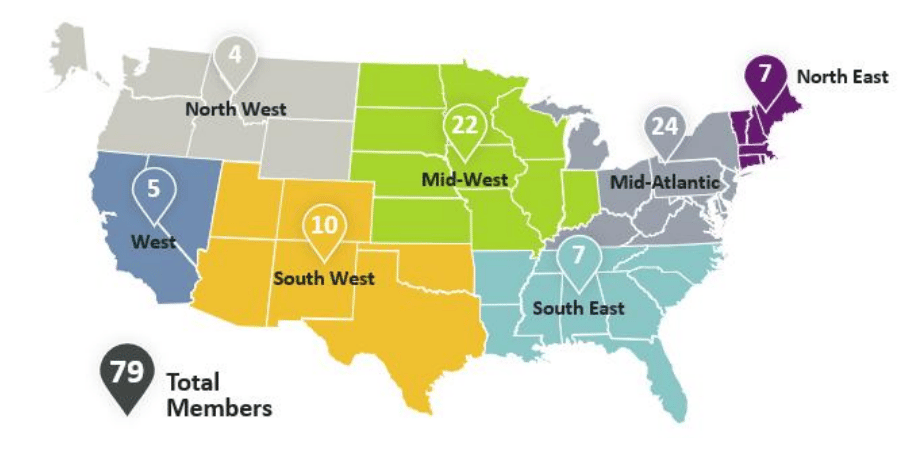
It feels so counterintuitive to me. Technology companies tend to be analytically driven, comfortable with risk, and oriented toward investments that require upfront work for long-term returns. Yet when it comes to health benefits, the default is almost universally the fully insured path. It is one of the clearest examples I have encountered of a hugely valuable solution going criminally unnoticed because it has never been translated into terms the audience actually speaks.
The Knowledge Gap Is the Real Problem
There is a saying among captive professionals: "When you have seen a captive, you have seen a captive." The point being: every program is genuinely different and the experience of one does not transfer cleanly to another. And I heard it more than once. I found it funny, because in the world I came from, if a client had seen a captive, they had literally only ever seen one.
But it points directly to the real problem. The people who understand captives best and the people deciding whether to use them almost never speak the same language. And very few people are positioned to translate between them without a meaningful conflict of interest.
The cost of doing nothing, or of choosing the wrong program, has never been higher. Checking a box with a captive quote is not a strategy. There are seven-figure implications over a multi-year commitment, and picking the wrong program, or the right one for the wrong reasons, produces outcomes that are difficult to undo. This requires real analysis.
What I Believe After My Research
Nobody should walk away from this expecting to save 20% in year one. Captives are a structure you move into that gets better every year you stay in it.
The year-one math looks modest. You stop paying the carrier margin on predictable spend, you get a surplus return from the captive pool, and depending on your program and your own claims performance, you likely come out a few points ahead of what fully insured would have cost. What matters is what happens in year two, year three, and five years in.
In a fully insured plan, you end every year with a renewal number and nothing else. No data you can act on, no leverage you built, no foundation for next year to improve on. The cycle resets. The carrier keeps what they learned about your population. You start from scratch, and the premium goes up.
In a captive, that cycle breaks. You have your data. You know what drove cost last year. You can identify which members are heading toward expensive episodes and get ahead of them. You can measure whether your cost containment programs are working. Every year you do that, your population performs a little better. Every year it performs a little better, your surplus grows. The cost of care starts to bend against a fully insured equivalent that compounds meaningfully forever.
Group captive programs are getting more competitive and widely available. The technology around claims management, cost containment, and proactive member guidance is improving quickly. And in a world where AI is making data analysis faster and more accessible than ever, being in a structure where you actually own your data is becoming increasingly valuable.
Taking back control is where it starts. The savings, the strategy, and the better outcomes for your employees all follow from that.
If you want to understand what the right fit looks like for your organization, I am happy to help. We provide proprietary program analysis, spend forecasting with probability modeling, and ongoing support to make sure the program you choose actually delivers on what it promises. There is no cost to you. Reach me at [email protected] or through the form on our site.

